Lymphaticovenous Anastomosis
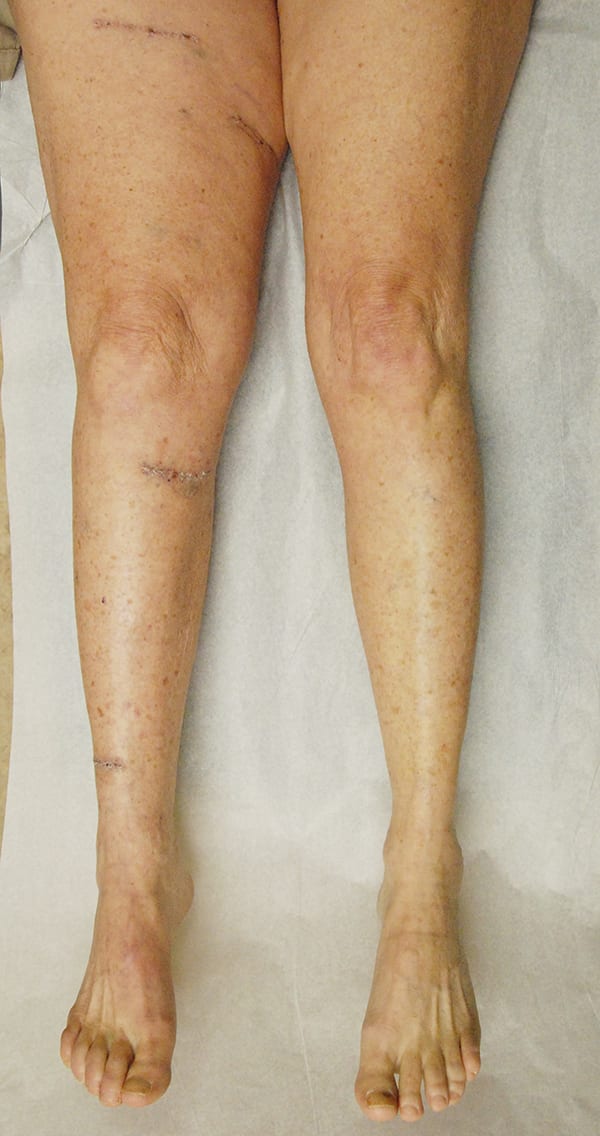
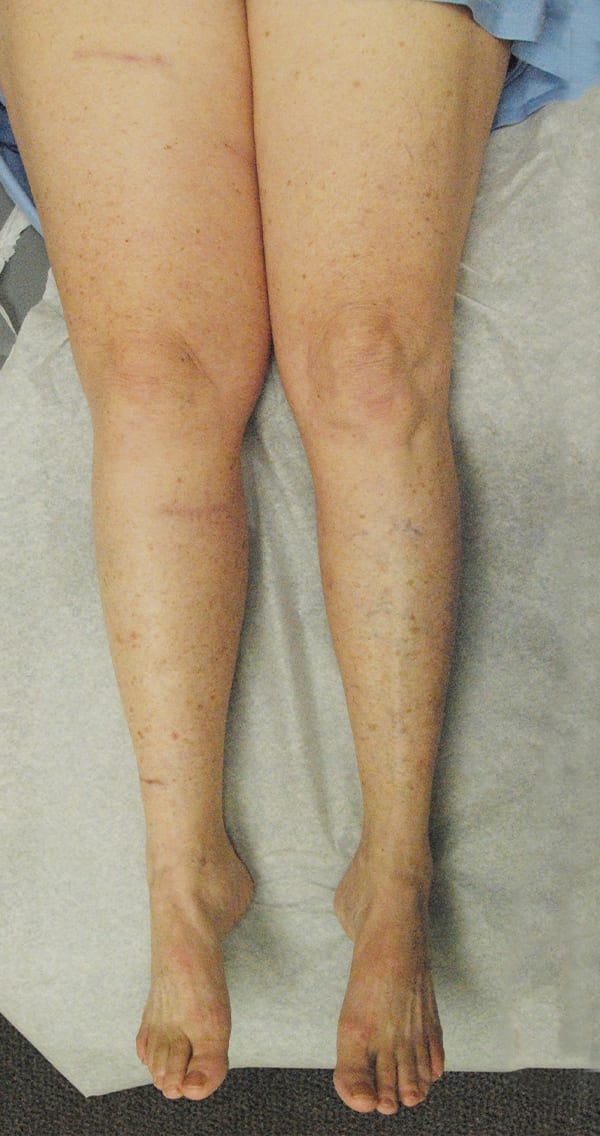
Lymphaticovenous anastomosis (LVA) surgery is part of the Granzow SystemSM of lymphedema treatment. LVA surgery is the least invasive when compared to other lymphedema surgeries with the fastest recovery. Published studies by Dr. Granzow and others have shown that LVA surgery has significantly decreased or eliminated the need for compression garments and therapy in his lymphedema patients.
LVA describes a method of directly connecting the lymphatic vessels in the affected area of the body to the tiny veins nearby. This allows the excess lymphatic fluid to drain directly into the vein and be returned to the body’s natural circulation.
An Improved Surgical Technique
Lymphaticovenous anastomosis (LVA) surgery uses superfine microsurgery, or “supermicrosurgery”, to connect lymphatic channels in the affected limb to nearby veins. These connections create additional outflow pathways to drain excess lymph fluid. Lymphatic vessels are tiny, typically ranging from 0.1 mm to 0.9 mm in diameter, and the superfine sutures used are only slightly larger than the thickness of a single strand of hair. LVA surgery uses specialized techniques, superfine instruments and the highest power operating room microscopes. The level of surgical skill required to identify the lymphatics, carefully separate them from the often severely scarred surrounding tissues and properly connect them to appropriate veins is among the highest in any surgical field.
As with VLNT surgery, LVA surgery works best for patients with stage 0 or stage 1 lymphedema, where fluid accumulation causes swelling. Dr. Granzow and his team carefully assess each patient to determine the best treatments for each individual case.
2-Stage Technique for Patients with Stage 2 Lymphedema
When properly used as part of a complete lymphedema surgery system, such as the Granzow SystemSM, LVA can effectively reduce the need for compression garments and lymphedema therapy even in patients with stage 2 lymphedema. In these patients with advanced lymphedema disease, Granzow SAPLSM surgery is used first to remove the excess pathologic lymphedema solids. After healing is complete, LVA and VLNT surgeries can be used to further decrease symptoms and lymphatic fluid accumulation. Dr. Granzow pioneered this use of VLNT and LVA surgery after Granzow SAPLSM surgery to successfully and consistently treat these patients.
To learn more about the Lymphaticovenous anastomosis (LVA) surgery, contact our Center of Excellence to schedule a consultation.